Skin Health & the DUTCH Test
McKenzie Mescon, ND
The DUTCH test can be useful in assessing our patients with skin concerns. Total androgen levels, androgen metabolism, the cortisol picture, and organic acid markers all tell us about the drivers for skin problems. There are also cases where DUTCH Test results do not show obvious patterns associated with skin health. In this article, we will examine how the DUTCH Test can guide our assessment of skin conditions, both through what is clear in the results, and by thinking dynamically about what is not. Factors beyond DUTCH testing that influence skin health include skin barrier function, medications, genetics, food sensitivity, thyroid function, nutrient status, the microbiome, and more.
Optimizing the Skin Barrier
The skin barrier is the place to begin when treating skin conditions. Optimizing skin barrier function involves hydrating, moisturizing, and reducing inflammatory triggers. While working to identify the underlying causes contributing to skin disease, start with healing the skin at the surface.
Review the topical products a patient is using regularly, such as soaps, exfoliants, and cleansers. In this current age of skincare maximalism with multi-step routines, a patient may not realize that their efforts at improving their skin are exacerbating inflammation and contributing to skin barrier dysfunction. Treatment of the skin barrier should focus on the following considerations:
- Using gentle cleansers and avoiding volatile oils or acids
- Encouraging proactive skin barrier protection with SPF and judicious sun exposure
- Moisturizing with ceramide-rich products following a shower or bath when the skin is still damp to help repair the skin barrier1
- Drinking an adequate amount of water and using a vaporizer/humidifier during dry months
- Eating foods that support a healthy microbiome
- Employing stress-management techniques
- Supplementing with approximately 2,200mg of flaxseed oil daily has been shown to support the skin barrier2
Analyzing DUTCH Test Results
Once the patient has started this boring but important work on the skin barrier, it is time to explore other underlying causes for the skin condition. The following table outlines findings on DUTCH test results that can guide clinical thinking in skin conditions.
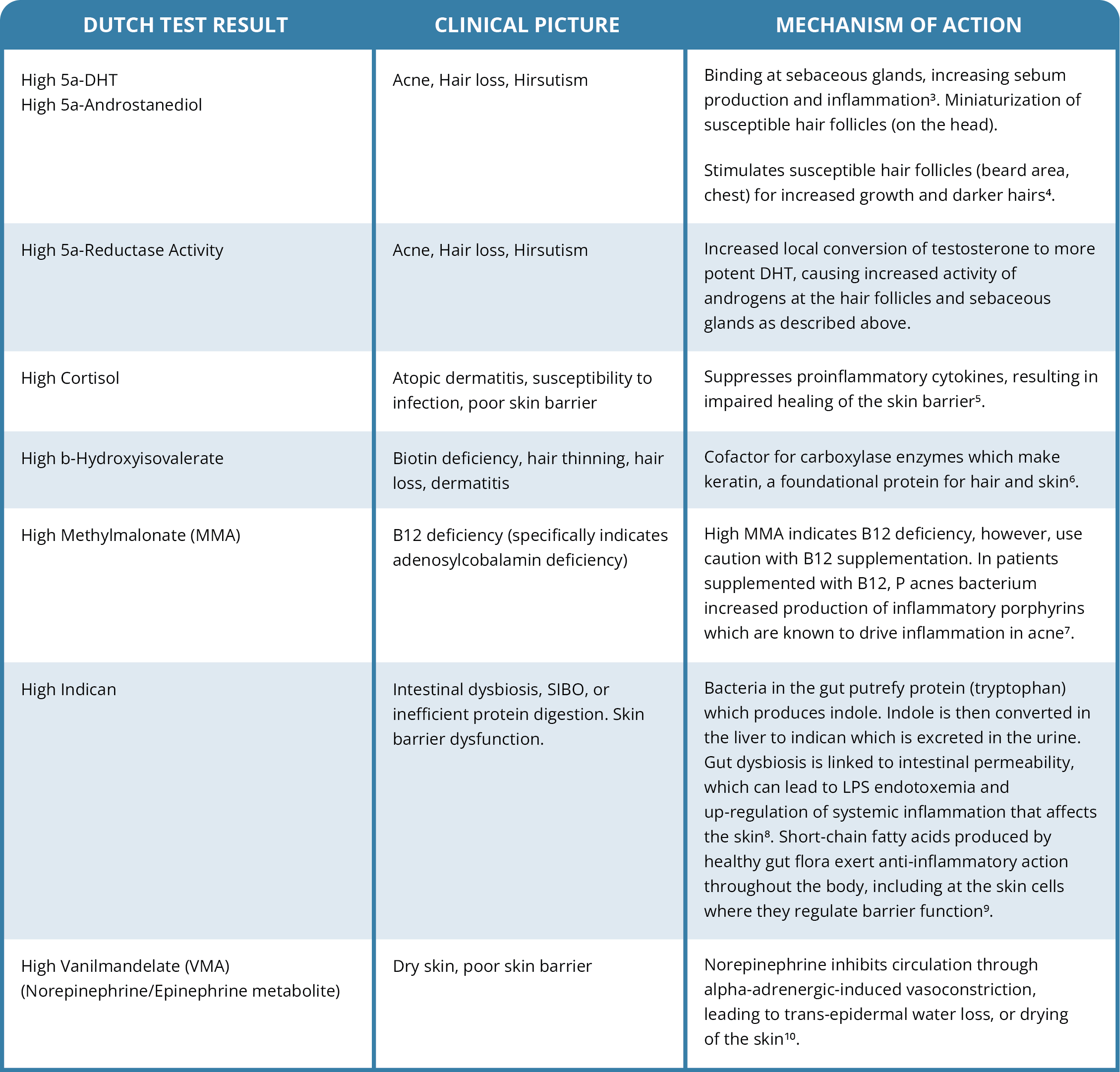
Imagine that the DUTCH Test of your patient with acne comes back with androgens (e.g., testosterone, 5a-DHT, 5a-Androstanediol, etc.) in the normal range, balanced 5a-reductase activity, a beautiful cortisol curve, a normal cortisol-clearance rate, and perfect OATs. I want every provider to know that this happens! While this can be frustrating for providers and patients, it provides actionable information; you can rule out many things. When there are no obvious causes at which to direct our treatment, it is time to go back to the chart notes and consider the patient. What makes the skin condition worse? What makes it better? What treatments has the patient tried that have worked? And what did not?
If a skin condition is worse during a particular phase of the menstrual cycle, consider the natural fluctuation of hormones during the month. Estrogen and progesterone normally decline before and stay low during menses. While androgen levels may be normal (hormone panels are often normal in acne patients), during menses there is not much estrogen or progesterone around to out-compete the androgens at the receptors. This is why many women experience acne during menses. Tending to the skin barrier in general may help improve resilience to the relative androgen-dominance of thismenstrual phase of the cycle. A few topical tools for reducing androgen-driven acne include:
- Topical green tea extract was shown to reduce inflammatory and non-inflammatory acne lesions11
- Topical or oral spironolactone blocks androgen activity in the skin and can be used in androgen-driven hair loss as well
- Twice daily spearmint tea intake showed a significant reduction in serum free and total testosterone levels over 30 days, with these patients reporting a subjective reduction in hirsutism12
In a patient whose skin condition improves when pregnant, consider the fact that the immune system down-regulates in pregnancy. Estrogen levels rise in pregnancy, and estrogen is supportive of healthy tissues, including the skin. On the other hand, if a patient’s skin condition worsens in late perimenopause or at the onset of menopause, the decline in tissue-nourishing estrogen may be driving skin barrier dysfunction. Hormone replacement may improve this patient’s skin condition.13
In a patient whose skin improves on birth control, consider how the suppression of hormones estrogen and progesterone, and their cycling, has created a stable state. The natural fluctuation of hormones during the cycle may contribute to inflammation or stress which may impact the skin barrier.
In the patient whose skin condition fluctuates, or improves with regular exercise and good sleep, consider the stress response. At the time of DUTCH testing, the patient’s sleep and exercise may have been optimal, and so the cortisol picture looks great. But the cortisol picture may change when mental health declines, the patient stops exercising regularly, or when sleep habits falter. Increased pituitary signaling to the adrenal gland in response to stress may also increase DHEA levels, and, being in the androgen family of hormones, DHEA can drive acne.14
If certain foods worsen a skin condition, food elimination may be an option for treatment. But socioeconomic status, social preferences, nutrition literacy, and anxiety can all be barriers to successful treatment with this method15 and care should be used in patients with a lived experience of an eating disorder. Insulin can be a driver for skin conditions such as acne,16 so assessment of both the glycemic load of the offending food and the patient’s insulin sensitivity can bring clarity to food triggers.
An alternative to removing foods from the diet is examining gut health. A dysfunctional gut microbiome can drive systemic inflammation, which may contribute to skin barrier dysfunction.17 The skin microbiome itself can also be a driving factor for inflammation that contributes to symptoms such as atopic dermatitis.18 The microbiome may be aberrant if antibiotic medications (oral or topical) have helped with a skin condition. Many antibiotics also have anti-inflammatory properties, and reducing inflammation may also have helped the skin condition.
If topical steroids help the skin condition, there is inflammation-driven skin barrier dysfunction. Topical steroids suppress immune activity, therefore calming reactivity. It is very hard to heal in a state of constant inflammation. Herein lies the argument for the judicious use of topical steroids, in combination with good barrier healing strategies, in the treatment of conditions such as eczema. A quick reminder here that topical steroid use can impact DUTCH test results.
If a patient’s acne improved on isotretinoin, (Accutane, a vitamin A analog) or has failed to improve with the addition of dietary or supplemental beta-carotene, the patient may have a genetic SNP in their beta-carotene 15,15’ monooxygenase 1 (BCM01) enzyme. This enzyme converts beta-carotene into its retinol form,19 retinoic acid, which modulates the immune response in the skin.20 This SNP may be present in any patient who has persistent skin conditions involving dysfunctional skin barrier and turnover. Supplementing with the retinol form of vitamin A, rather than the beta-carotene form, is appropriate in these patients.
There are several things to consider in a patient experiencing hair loss that is not driven by androgenic activity or biotin deficiency.
- Thyroid Function: Skin is a significant target for thyroid hormones. In hypothyroidism, cell division is impeded, leading to hair loss in 33% of hypothyroid patients. Repleting thyroid hormone often resolves hair loss in these patients, except in those with long-term hypothyroidism with atrophy of hair follicles.21 In hyperthyroidism, the inflammation generated by reactive oxygen species may contribute to hair loss in 50% of hyperthyroid patients, though the exact mechanism is unknown.22
- Iron Status: Iron deficiency can also be a cause of hair loss and can be assessed with serum testing.
- Stress: Telogen effluvium is a temporary hair loss caused by a stressful shock such as illness or a severe stressful event. Telogen effluvium typically resolves on its own.
- Autoimmunity: Alopecia areata is a chronic inflammatory autoimmune disorder causing hair loss with small, round, smooth patches on the scalp, face or body.
- Other causes for hair loss include traction alopecia and scarring alopecia.
No matter the skin condition, the underlying cause, or the treatment strategy, treating skin conditions starts with addressing the skin barrier. As the skin barrier heals, triggers may make themselves more apparent, and the clinical picture becomes clearer. Our patients will thank us if we treat their skin barrier while we work on the underlying causes. DUTCH testing is a useful tool for assessing contributing factors to skin conditions, even when the outcome is a normal test result that allows you to rule out the primary suspects.
References
- Yong TL et al. Ceramides and Skin Health: New Insights. Experimental Dermatology. 2025.
- Neukam N et al. Supplementation of flaxseed oil diminishes skin sensitivity and improves skin barrier function and condition. Skin Pharmacol Physiol. 2011;24(2):67-74.
- Elsaie M. Hormonal treatment of acne vulgaris: an update. Dovepress. 2016;2016(9):241-248.
- Grymowicz M et al. Hormonal Effects on Hair Follicles. International Journal of Molecular Sciences. 2020;21(15):5342.
- Maarouf M, et al. The impact of stress on epidermal barrier function: an evidence-based review. British Journal of Dermatology. 2019;181(6):1129-1137.
- Cervantes A, et al. Biotin Deficiency. StatPearls. September 14, 2025
- Kang D, et al. Vitamin B12 modulates the transcriptome of the skin microbiota in acne pathogenesis. Science Translational Medicine.2015;7(293):293ra103.
- Zhao M, et al. Immunological mechanisms of inflammatory diseases caused by gut microbiota dysbiosis: A review. Biomedicine and Pharmacotherapy. 2023;164
- Xiao X, et al. The role of short-chain fatty acids in inflammatory skin diseases. Frontiers in Microbiology. 2023;2(13):1083432.
- Maarouf M, et al. The impact of stress on epidermal barrier function: an evidence-based review. British Journal of Dermatology. 2019;181(6):1129-1137.
- Kim S, et al. The effects of green tea on acne vulgaris: A systematic review and meta-analysis of randomized clinical trials. Phytotherapy Research. 2021;35(1):374-383.
- Grant, P. Spearmint herbal tea has significant anti-androgen effects in polycystic ovarian syndrome. A randomized controlled trial. Phytotherapy Research. 2010;24(2):186-188.
- Stevenson S, et al. Effect of estrogens on skin aging and the potential role of SERMs. Clinical Interventions in Aging. 2007;2(3):283-297.
- Palatsi R, et al. Pituitary Function and DHEA-S in Male Acne and DHEA-S, Prolactin and Cortisol before and after Oral Contraceptive Treatment in Female Acne. Acta Dermato-Venereologica. 1986;66(3):225-230.
- Malone J C, Daley S F. Elimination Diets. StatPearls. January 9, 2024.
- Hasrat N, et al. The Relationship Between Acne Vulgrais and Insulin Resistance. Cureus. 2023;15(1):e34241.
- Hou B, et al. Skin and gut microbiome in atopic dermatitis: Mechanisms and therapeutic opportunities. Pediatric Allergy and Immunology. 2025;36(12):e70265.
- Hou B, et al. Skin and gut microbiome in atopic dermatitis: Mechanisms and therapeutic opportunities. Pediatric Allergy and Immunology. 2025;36(12):e70265.
- Lindqvist A, et al. Biochemical Properties of Purified Recombinant Human B-Carotene 15,15’-Monooxygenase. Journal of Biological Chemistry. 2002;277(26):23942-23948.
- Roche F, et al. Illuminating the Role of Vitamin A in Skin Innate Immunity and the Skin Microbiome: A Narrative Review. Nutrients. 2021;13(2):302.
- Hussein R, et al. Impact of Thyroid Dysfunction on Hair Disorders. Cureus. 2023; 15(8):e43266.
- Hussein R, et al. Impact of Thyroid Dysfunction on Hair Disorders. Cureus. 2023; 15(8):e43266.
TAGS
General Health
General Hormone Health
Androgens (Testosterone/DHEA)
Inflammation
Acne