You Need Free Cortisone and Metabolized Cortisol to Evaluate HPA Axis Health
Kelly Ruef, ND
You Need Free Cortisone and Metabolized Cortisol to Evaluate HPA Axis Health
by Kelly Ruef, ND
Not all cortisol tests are created equal. For your patient complaining of anxiety and fatigue, a standard test kit that measures free cortisol levels throughout the day might not be enough.
If you only look at the diurnal rhythm of free cortisol you are likely missing the big picture. You also need to consider metabolized cortisol and free cortisone when evaluating HPA axis health, and here’s why.
What is metabolized cortisol?
Metabolized cortisol on the DUTCH Test is the sum of the most abundant cortisol metabolites, a-THF, b-THF, and b-THE. It is the best marker for assessing the total production of cortisol by the adrenal glands. Unfortunately, free cortisol and free cortisone can only give us an idea of free levels in circulation , not total production, and this is why it is vital to measure cortisol metabolites. You might be surprised to know that a person’s total production of cortisol can be greatly different from their total free cortisol and cortisone in circulation. We will discuss this concept in more detail below.
What is free cortisone?
Free cortisone is the cortisol in the free form that is inactive. It’s inactive because it cannot act on receptors and thus does not exert any effects on the body.
Why test free cortisone in addition to free cortisol?
When measuring cortisol in the urine or saliva, one must measure free cortisone in addition to free cortisol.
Why? The short answer is that a portion of the free (active) cortisol that enters the kidneys or salivary glands from circulation gets deactivated to free (inactive) cortisone by an enzyme known as 11b-HSD2. Thus, some of the free cortisol that was in the blood shows up as free cortisone in the urine and saliva.
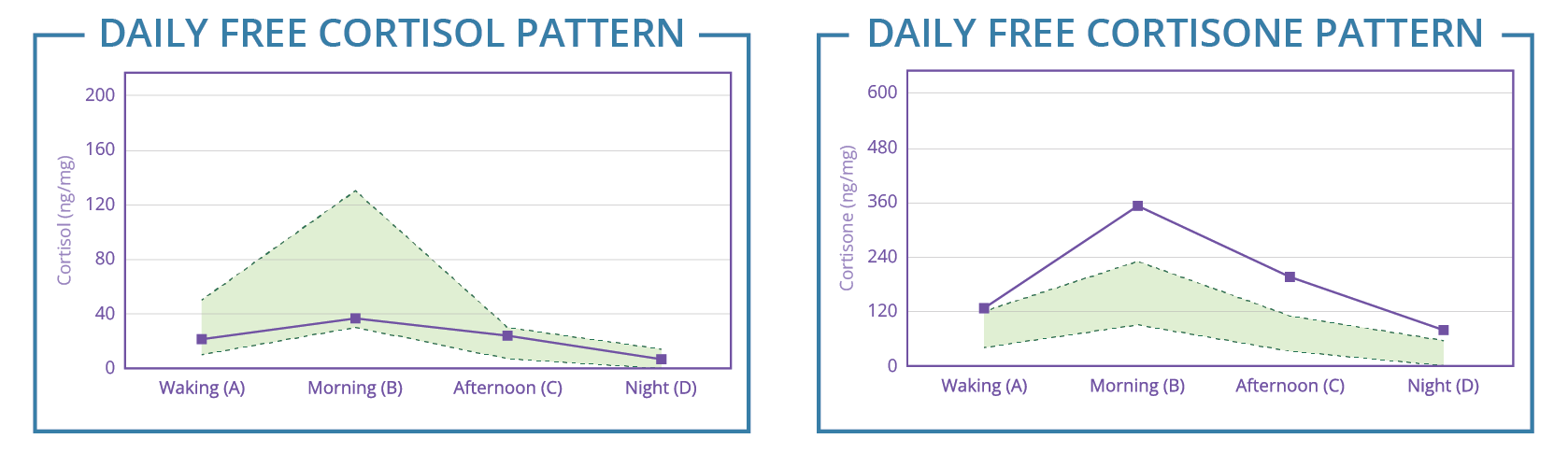
If you only tested free cortisol’s diurnal rhythm, you could be missing the mark. Consider the example below. The daily free urinary cortisone pattern is elevated, however, the daily free urinary cortisol pattern is on the low end of the range. If you only tested the free cortisol, you might incorrectly treat for low cortisol.
Instead, you realize that the patient’s free cortisol in the bloodstream probably looks more like the urinary free cortisone pattern, or somewhere in between the two patterns. With the added free cortisone data, you can consider targeting your treatments toward lowering cortisol.
How do free cortisone and metabolized cortisol provide more insight into a patient’s HPA axis health?
As stated above, free cortisone enables you to have a more accurate view of free (active) cortisol levels in circulation. Additionally, the metabolized cortisol enables you to get a better idea of the total amount of cortisol that was produced by the adrenal glands, and it enables you to calculate the cortisol clearance rate (CCR).
The CCR tells you how quickly cortisol is metabolized and cleared out of circulation. It can be estimated by comparing the total free cortisol and cortisone with the metabolized cortisol on a DUTCH report. When metabolized cortisol is relatively lower than the total free cortisol and cortisone, the CCR is said to be slow . Oppositely, when metabolized cortisol is relatively higher than the total free cortisol and cortisone, then the CCR is said to be fast . Evaluating the CCR can improve a treatment plan because a slow CCR and a fast CCR are associated with various conditions. To explain this further, let’s look at three examples.
DUTCH Test Pattern: Fast CCR
In the example below, plenty of cortisol is being produced by the adrenals (metabolized cortisol is on the high end of the range), however, the free cortisol and cortisone in circulation are on the low end of the range. This is likely because cortisol is being metabolized and cleared from circulation quickly. If you only tested the free cortisol diurnal rhythm, then you may incorrectly treat for low cortisol.
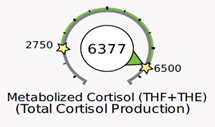
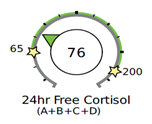
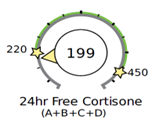
A fast CCR as seen above may be associated with obesity, inflammation, blood sugar and insulin dysregulation, hyperthyroidism (or excessive thyroid medication), and long-term stress. In obesity, adipose tissue sequesters cortisol, which in turn may further increase cortisol production (metabolized cortisol).
DUTCH Test Pattern: Slow CCR
In the example below, there is not much cortisol being produced by the adrenals (metabolized cortisol is below the range), however, the free cortisol and cortisone in circulation are within range. This is likely because cortisol is being metabolized and cleared from circulation slowly. If you only tested the free cortisol diurnal rhythm, then you may incorrectly assume that cortisol levels are normal.

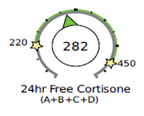
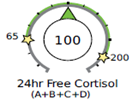
A slow CCR as seen above may be associated with things that tend to lower the overall metabolic rate, such as hypothyroidism (or insufficient thyroid medication), low-calorie intake (anorexia), low bile acid, and poor liver and mitochondrial function.
DUTCH Test Pattern: Normal CCR
In the example below, an elevated total amount of cortisol is being produced by the adrenals (metabolized cortisol is above range). The free cortisol and cortisone in circulation tell the same story of excess cortisol. This person has a normal cortisol clearance rate because the metabolized cortisol dial is pointing in the same direction as the 24hr free cortisol and free cortisone dials—they are all above range.
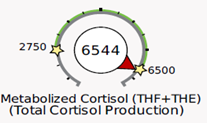
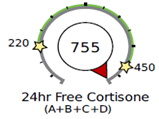
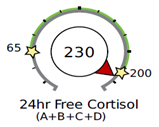
Note that a normal CCR does not automatically rule out conditions that tend to slow down or speed up cortisol metabolism, as outlined above.
More Comprehensive HPA Axis Monitoring with DUTCH
It is easy to see that DUTCH testing offers a more comprehensive look into the HPA axis. The DUTCH Complete, DUTCH Plus, and DUTCH Adrenal panels all include free cortisol and free cortisone patterns, along with metabolize cortisol, so that you can take your HPA axis health assessment to the next level.
If you’d like to learn more, please refer to pages 112-117 of the DUTCH Interpretive Guide for more details on free cortisone, metabolized cortisol, and the cortisol clearance rate (CCR). If you don’t already have access to the DUTCH Interpretive Guide, you can download it directly from the provider portal!
References
- Blair J, et al. Salivary cortisol and cortisone in the clinical setting. Curr Opin Endocrinol Diabetes Obes. 2017 Jun;24(3):161-168.
- Perogamvros I, et al. Salivary cortisone is a potential biomarker for serum free cortisol. J Clin Endocrinol Metab. 2010 Nov;95(11):4951-8.
TAGS
Cortisol
Cortisol Metabolism
Women's Health
Men's Health