Supporting Perimenopause with the DUTCH Test
Hilary Miller, ND
Women in their late 30s and early 40s are undoubtedly experiencing shifting hormones. Hormone changes preceding menopause begin even before noticeable changes in the menstrual cycle. As a result, symptoms associated with perimenopause can be dismissed or attributed to nonspecific effects of aging. Doctors and healthcare providers can fail to recognize symptoms of hormone shifts because they have little guidance on recognizing or testing in perimenopause. Testing in perimenopause can be difficult to interpret, given the high variability of this phase in life. The DUTCH test has panels that offer solutions to testing in this age group, looking in-depth at sex and adrenal hormones, the two major systems that impact women during this stage.
Perimenopause is a challenging phase of life and is often underestimated. While some women will seek out information from their providers, many may ignore their symptoms or attribute them to stress or aging. Providers may recognize a pattern of complaints but fail to connect the symptoms with sex hormones. This is likely due to minimal menstrual cycle changes early in this process. Before they notice cycle changes, women often report changes in mood, sleep, weight, energy, and cognition. Noticeable changes in the length and quality of the menstrual cycle occur after hormone changes are already occurring.
In 2021, a study by Coslov et al.(1) was published out of the Women Living Better Survey. 1,436 women aged 35-55 were staged according to reproductive aging status and answered an 82-question symptom survey. The study compared the quality of life in the late reproductive stage* (LRS) to the menopausal transition** (MT). Their striking finding was that women in the LRS experienced many similar symptoms that interfered with their lives at similar levels to women in the MT, and many were surprised this was happening so early. They expressed they "...did not anticipate these symptoms until they were 50 years old." [Coslov 2021] The implication for clinicians is clear: changes in sex hormones should be considered as a potential root cause for numerous changes in health and well-being in women of this age group, regardless of whether their cycles have changed.
*The late reproductive stage or LRS is a stage of reduced fertility and altered ovarian hormone output but cycles are still regular.
**The menopausal transition or MT is the transition stage where cycles get increasingly irregular and ovarian function declines to menopausal levels.
Although the stages of perimenopause have been studied and defined, such as in the Stages of Reproductive Aging Workshop (STRAW)(2), doctors can’t use this information to predict when the next phase will occur. The STRAW criteria only serves to identify either a woman's current stage or as with diagnosing menopause, can stage retrospectively. Our first diagram below shows expected hormone changes, starting with the LRS, which typically occurs for women in their late 30s and early 40s. Starting sometime after 40, women move into the second phase of the diagram with slightly lower progesterone and slightly higher estrogen which advances to erratic estrogen, both high and low. These hormone changes have dramatic impacts on quality of life. Lower progesterone is commonly associated with poor sleep, irritability, anxiety, and heavier menses. Higher estrogen is associated with breast tenderness, emotional lability, agitation, and also heavier menses. By the late MT, women are experiencing low progesterone AND low estrogen, associated with hot flashes, night sweat, vaginal dryness, insomnia, and depression.
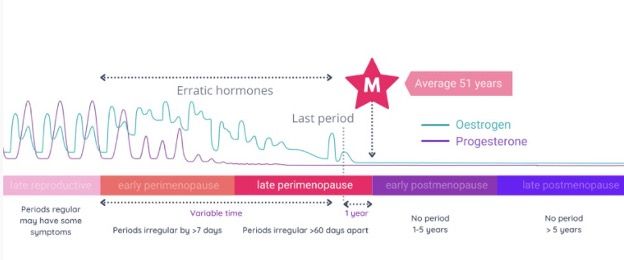
Challenges with lab testing can lead providers to often offer symptomatic support without considering the impact of ovarian hormones. This approach has some benefits because adopting lifestyle changes can significantly improve hormonally driven symptoms for many women. Unfortunately, symptomatic approaches can include medications that don’t address the root cause such as SSRIs and zolpidem (a sleep medication). Having a full understanding of the changes in hormone levels can optimize care.
Conventional lab testing during this phase is inherently difficult. In the graph below, which shows a typical healthy reproductive cycle, you see two arrows pointing down at the points in the cycle that are traditionally tested.
On the left of the chart below, testing estradiol (E2) and follicle stimulating hormone (FSH) in the early follicular phase can identify ovarian dysfunction: high or high end FSH in the early follicular phase can indicate follicular aging. If E2 is low while FSH is high, follicular aging is more advanced.
On the right of the chart below, testing E2 and progesterone (P) in the luteal phase can identify symptomatic hormone imbalance. Both high or low E2 can indicate ovarian aging and cause many hormone imbalance symptoms. A decrease in P from the patient's previous levels can cause symptoms just as much as a low or low-end P, even if the decrease shows a value that remains within the luteal phase range. A common cause of early perimenopause symptoms is when P is on the low end of the luteal range or is frankly low.
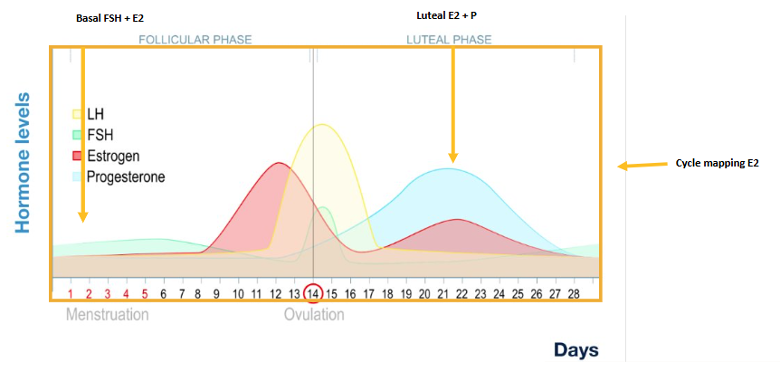
Via UCSF's Center for Reproductive Health
While looking at these two points (described above) is helpful, if you take the whole diagram, you'll see that the cycle is complex. Testing two single points fails to capture significant hormone impairments across the cycle for a given patient. You may already be thinking of another inherent problem with traditional testing: perimenopausal hormone cycles are sometimes unpredictable and irregular, so finding the right "day" of the cycle can be so challenging it can make test results impossible to interpret.
The diagram shows another testing option to the right. DUTCH Cycle Mapping is a map of estrogens and progesterone metabolites over a menstrual cycle, providing clarity for blind spots in traditional testing. Cycle Mapping can better identify the hormonal inputs to symptoms of perimenopause. Many perimenopausal symptoms can also be tied to stress, inflammation, nutrient deficiency, low melatonin, and other hormone changes of aging, which makes a Cycling Mapping combined with a one-day DUTCH test like the DUTCH Complete (DC) or the DUTCH Plus (DP) much more comprehensive .
Let's look at a case to demonstrate our point.
Lois is 39 years old with regular cycles that are 26-27 days long (used to be 28 days long). She reports:
- Mild: Hair loss, night sweats, and anxiety.
- Moderate to severe: Fatigue, heavy menses, tender breasts, nighttime waking, and migraines.
Below is a snapshot of her Cycle Mapping and DUTCH Plus Hormone Summary. We see significantly more about her hormones on the Cycle Mapping report than if we had tried a day 21 serum test. Her estrogen cascade is normal, with ovulation occurring a little earlier than typical on days 11-12. Her estrogens were in a normal range throughout the cycle. Her peak progesterone occurred on day 19 and was on the low end of the luteal range. On her DUTCH Plus we see the peak progesterone placed on the dial next to the same day's E2. The dials show relative estrogen dominance, confirmed by the low progesterone throughout the cycle on the Cycle Mapping report.
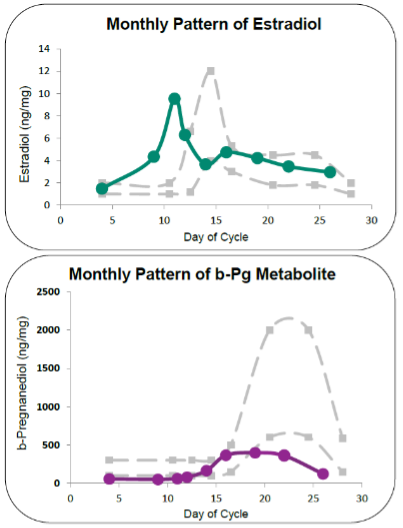
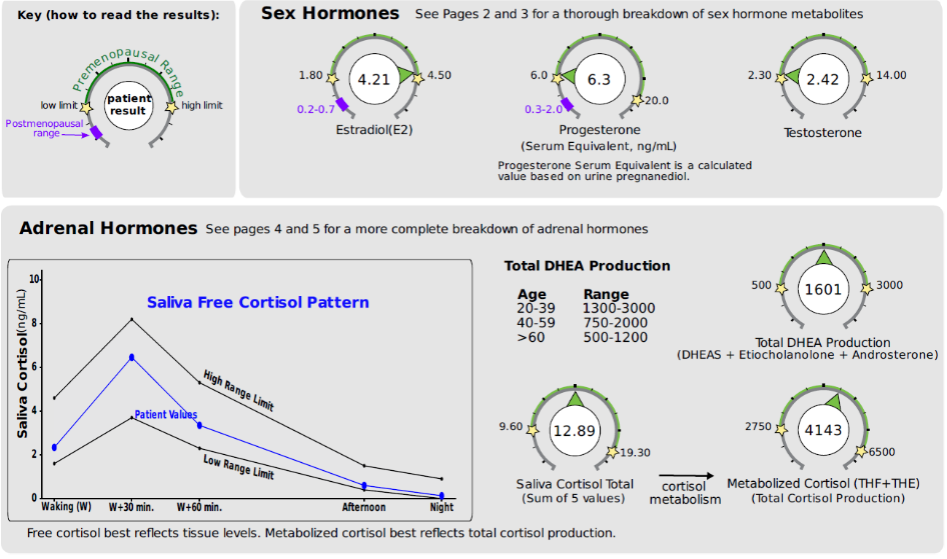
Lois' Cycle Mapping report gave us much more information than we would have had from testing one or two days of her cycle, as conventional testing dictates. We can also be assured we captured her peak progesterone since she tested multiple times in her luteal phase. We have the luxury of choosing the highest result to compare to her estrogen, showing a clear issue: low-normal progesterone.
Her testosterone is low for her age, but total DHEA is normal. She might consider testosterone therapy in the future, but most protocols suggest balancing estrogen and progesterone first. While her free and metabolized cortisol totals are normal, we see a high CAR at 176%, which could be contributing to her stress and night sweats. She might consider adaptogens and meditation for stress management.
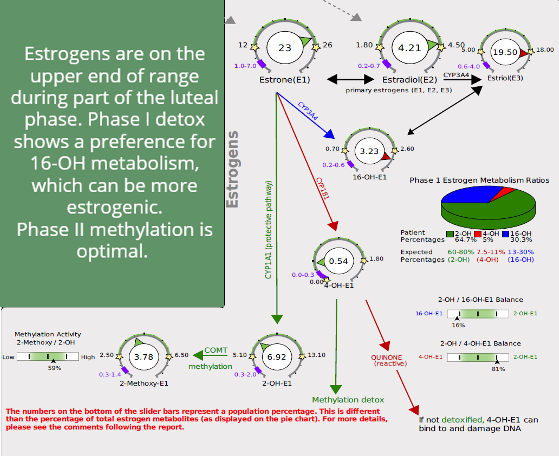
The DUTCH Plus shows her estrogen detox, androgens, cortisol, several nutrients, and neuro-related markers. Her phase 1 estrogen detox (below) favors 16-OH-E1, an estrogenic metabolite. She may see reduced breast tenderness and heavy menses by optimizing both her progesterone-to-estrogen ratio and her phase 1 detox. This might be a case for DIM, which a recent DUTCH peer-reviewed paper (link to DIM paper please) showed can lower parent estrogens and optimize the ratio of 2-OH to 16-OH-E1(3). She might also consider hormone therapy like progesterone-only therapy, which might balance out the effects of estrogen.
The Cycle Mapping and DUTCH Plus gave much more complete information about what could be causing her symptoms than conventional testing would have. Cycle Mapping simplifies the pitfalls of hormone testing in perimenopause, where timing and interpretation are challenging. In Lois' example, her cycles were relatively regular. This example highlights how, even in regular cycles, conventional testing might give only limited information. Cycle Mapping is even more helpful with irregular cycles where the ambiguous timing of sample collection can make interpreting results nearly impossible.
While perimenopause is a normal phase of life, women do not need to suffer through symptoms of hormone imbalance. Even when menstrual cycles are normal, hormone shifts may impact quality of life. Symptoms associated with menopause can be dismissed or linked to other life events, but hormone testing should be considered. DUTCH Cycle Mapping and one-day testing like the DUTCH Complete or Plus enhance the insight into perimenopause, a boon to providers looking to design actionable plans for perimenopausal women.
References:
1. Coslov N, et al. Symptom experience during the late reproductive stage and the menopausal transition: observations from the Women Living Better survey. Menopause. 2021;28(9):1012-1025.
2. Harlow SD, et al. Executive Summary of the Stages of Reproductive Aging Workshop + 10: Addressing the Unfinished Agenda of Staging Reproductive Aging. J Clin Endocrinol Met. 2012;97(4):1159-1168.
3. Newman M, et al. Exploring the impact of 3,3'diindolylmethane on the urinary estrogen profile of premenopausal women. BMC Complement Altern Med. 2024;24(405):1-10.
TAGS
Women's Health
Perimenopausal Women
Perimenopause
Estrogen and Progesterone
Low Progesterone
Laboratory Testing: In-Depth Look at DUTCH Urine Testing
Estrogen Detoxification
Estrogen Metabolism
Hormone Replacement Therapy (HRT)